
By Alyce Collins
Dentist, Louise Double (31) from Manchester, UK, but now living in Jersey, thought her pregnancy was going well after only having morning sickness early on, but after going into labour in June 2018 her health soon deteriorated.
After finally going into labour two weeks late, Louise required an assisted delivery because her baby’s heart rate was dropping quickly, so doctors needed to get her out immediately.

MDWfeatures / Louise Double
Following an epidural, Louise felt a pain in her ribs which midwives assumed was just labour pains. Although half an hour after delivery Louise insisted that she didn’t feel well as her skin began to turn yellow and her blood pressure was dropping quickly. Immediately after the delivery Louise was taken to intensive care where she was placed on dialysis.
Tests revealed that Louise’s liver was failing so she was put on dialysis to save her kidneys, and the decision was made to send her for specialist treatment, meaning Louise had to be sent on an emergency flight by the Royal Air Force in a helicopter to London to receive the specialist care required. She was put on the critical donor list meaning she would most likely receive the next one available in the country as she was the sickest person at that time.

MDWfeatures / Louise Double
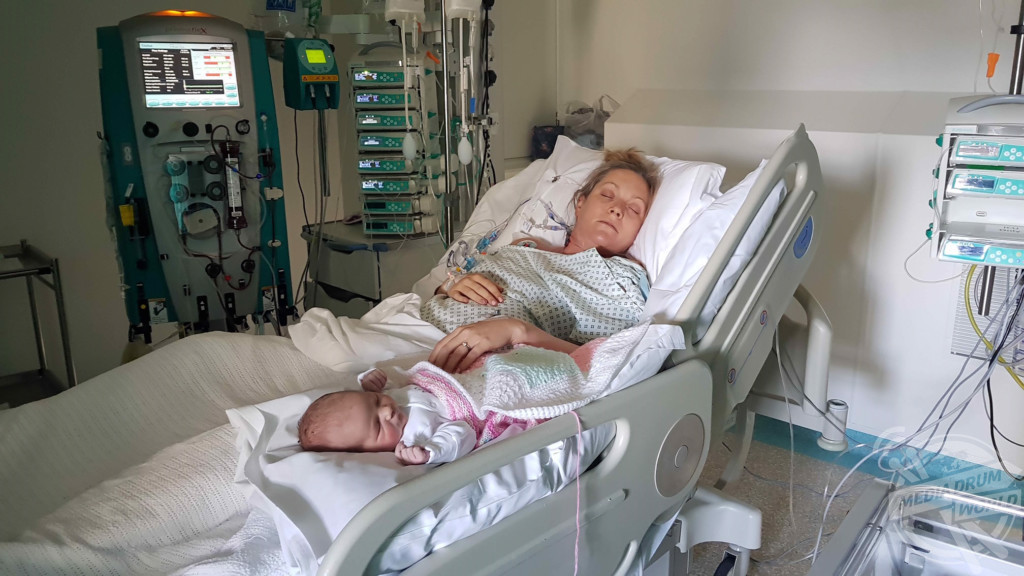
Louise spent the first month of her daughter, Amelia’s life in hospital in another country which was incredibly hard for both of them. Louise’s husband, Dave, flew to London, while Amelia stayed with relatives and friends, and was brought to London two weeks later.
Louise hopes to encourage more people to become organ donors after having her life saved from what doctors indicated was most likely HELLP syndrome, a rare syndrome that occurs in pregnant women and can cause organ failure, and in some cases death.

MDWfeatures / Louise Double
“Other than morning sickness for the first half of my pregnancy, it was fairly uneventful, and I was healthy,” said Louise.
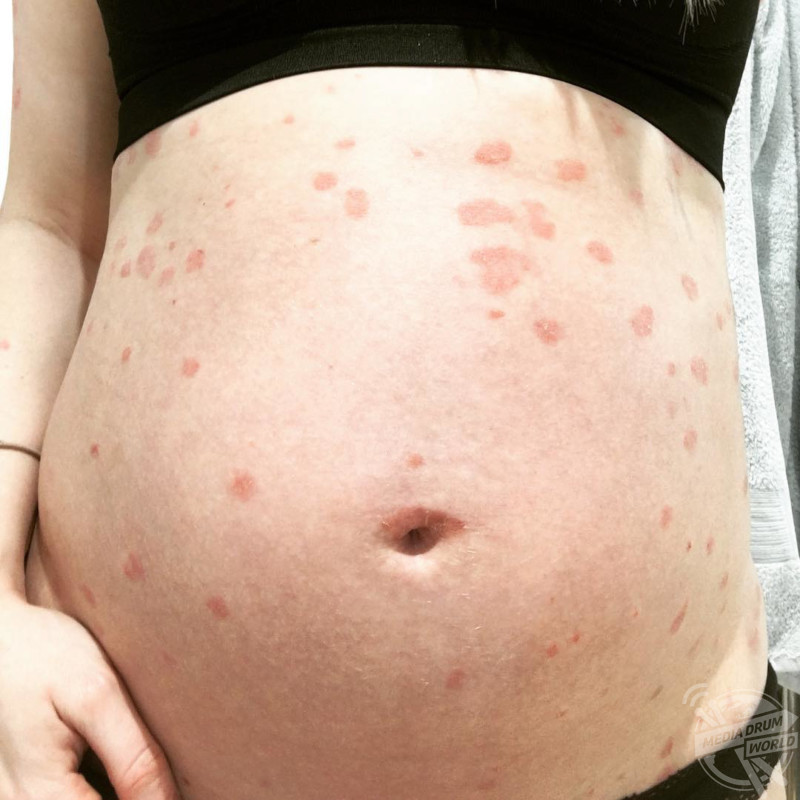
“I worked full time up until I was 38-weeks pregnant. I had severe psoriasis on my skin while I was pregnant which was very itchy. In hindsight this itching could have been a sign of the liver disease at the beginning.

MDWfeatures / Louise Double
“I went into labour and almost two days later ended up needing an assisted delivery as her heart rate was dropping when I pushed.
“After my epidural I was complaining of pain in my ribs, which was most likely a symptom of my liver failing. It was just assumed to be labour pains, but then 30 minutes after delivery I started to complain about feeling unwell and I started to turn a bit yellow.

MDWfeatures / Louise Double
“The team checked my blood pressure and platelets were getting dangerously low. I was then taken to intensive care in Jersey hospital. The doctors put me on dialysis and were speaking to some hospitals about where to send me for specialist treatment.
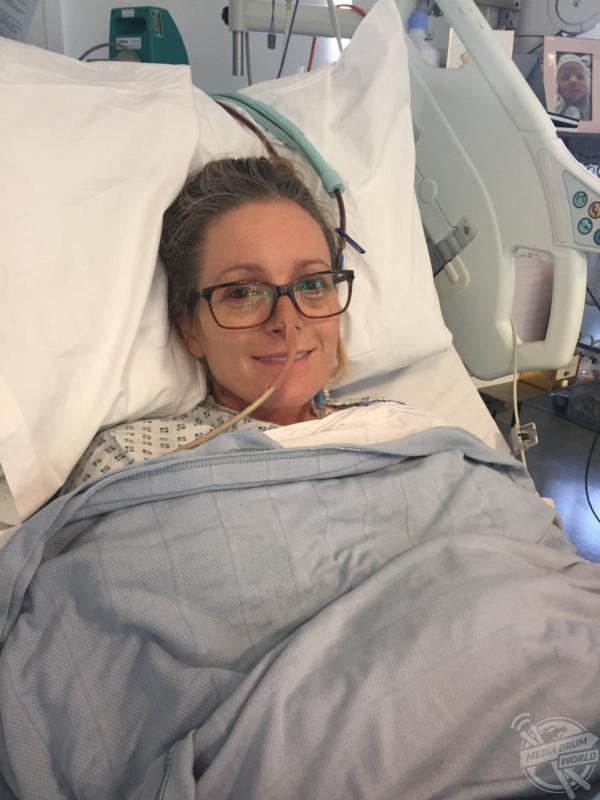
“The decision was to fly me over to King’s College Hospital two days later, via RAF helicopter. I remember being in a lot of pain in the helicopter, it was very scary. I have amnesia from moments after giving birth until waking up after my transplant.
MDWfeatures / Louise Double
“Doctors in both hospitals ran constant blood tests which showed my liver enzymes were very high, showing failure. The specialist at King’s College Hospital said it would have to be a transplant or most likely death.
“I was so lucky to have such wonderful care there. I was in the hospital for a month before returning home.

MDWfeatures / Louise Double
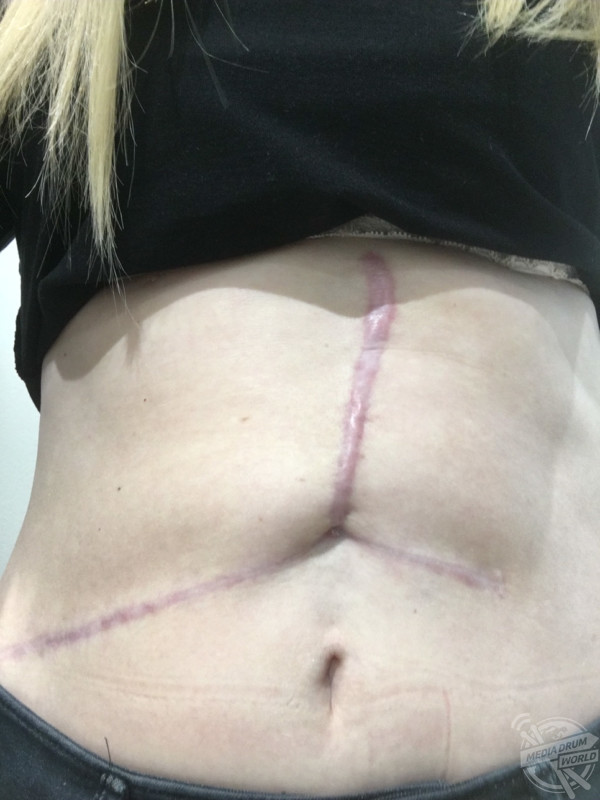
“My legs and arms suffered muscle wastage from two weeks in intensive care, my scar has taken a long time to heal and I’ve suffered some PTSD. During the liver failure I was so swollen that I went from a UK size 10 to a size 16.
“It was horrendous because instead of spending time with my new family, I was on my own in a room on a hospital ward.”

MDWfeatures / Louise Double
Doctors can’t be entirely sure what condition caused Louise’s liver failure, but tests indicate the likelihood of her condition being HELLP, which is known to cause complications with the liver during pregnancy.
HELLP refers to the features of the disease, including elevated liver enzyme levels and low platelet levels. Although other doctors suggested she could have contracted sepsis at the time of delivery which may have contributed to the liver failure.
MDWfeatures / Louise Double
“I will need blood tests to continually monitor whether my liver is showing any signs of failure or rejection in the future,” said Louise.
“At this point there is no way of 100 per cent confirming what went wrong, but most of the post-partum tests indicate that it was most likely HELLP.

MDWfeatures / Louise Double
“This was the best assumption the doctors came up with, but it wasn’t clear if it was entirely that or maybe sepsis at the time of delivery.
“HELLP is a rarer form of preeclampsia, which is interesting because my mother had preeclampsia when she carried me.

MDWfeatures / Louise Double
“It’s taken a long time to become physically stronger, at least five months. Sometimes I’m unable to pick Amelia up so I’ve needed someone to come over and help.
“I’m now on strong medication indefinitely to try and prevent rejection and my risk of infection and cancer is much higher now.
MDWfeatures / Louise Double
“I still can’t sit up properly as I was told not to do any abdominal exercise until things have fully healed and picking up my daughter is still difficult.
“I didn’t get to initially bond with my daughter because I was too preoccupied by being sick in hospital. Being separated and ill delayed me bonding with her, and not only were we apart but I wasn’t able to breastfeed which upset me.”

MDWfeatures / Louise Double
Louise also spoke about the importance of organ donation and making family members aware of your preferences, should anything ever happen. Louise herself learned the need for donors to come from all backgrounds to better improve the chances of finding matches.
“It’s important that donors are from all walks of life to create more chances of finding matches with all blood types, especially rare ones,” Louise said.

MDWfeatures / Louise Double
“It’s important to let your family know what your preference is and consider being on the donor list, should you lose your life. It’s a sensitive issue, especially with different cultures and religions, but organ failure can affect anyone at any time.
“I certainly never expected that I would be in this situation, so if you needed to be saved in a life or death situation, you should consider whether it’s morally okay to not be a donor.”
MDWfeatures / Louise Double
You can follow Louise by visiting @louise1358.






