By Rebecca Drew
THIS WOMAN was misdiagnosed with SCHIZOPHRENIA after psychosis kept her awake for TEN DAYS STRAIGHT and made her think her SISTERS WERE DEAD – but her symptoms were actually caused by a rare autoimmune disorder.
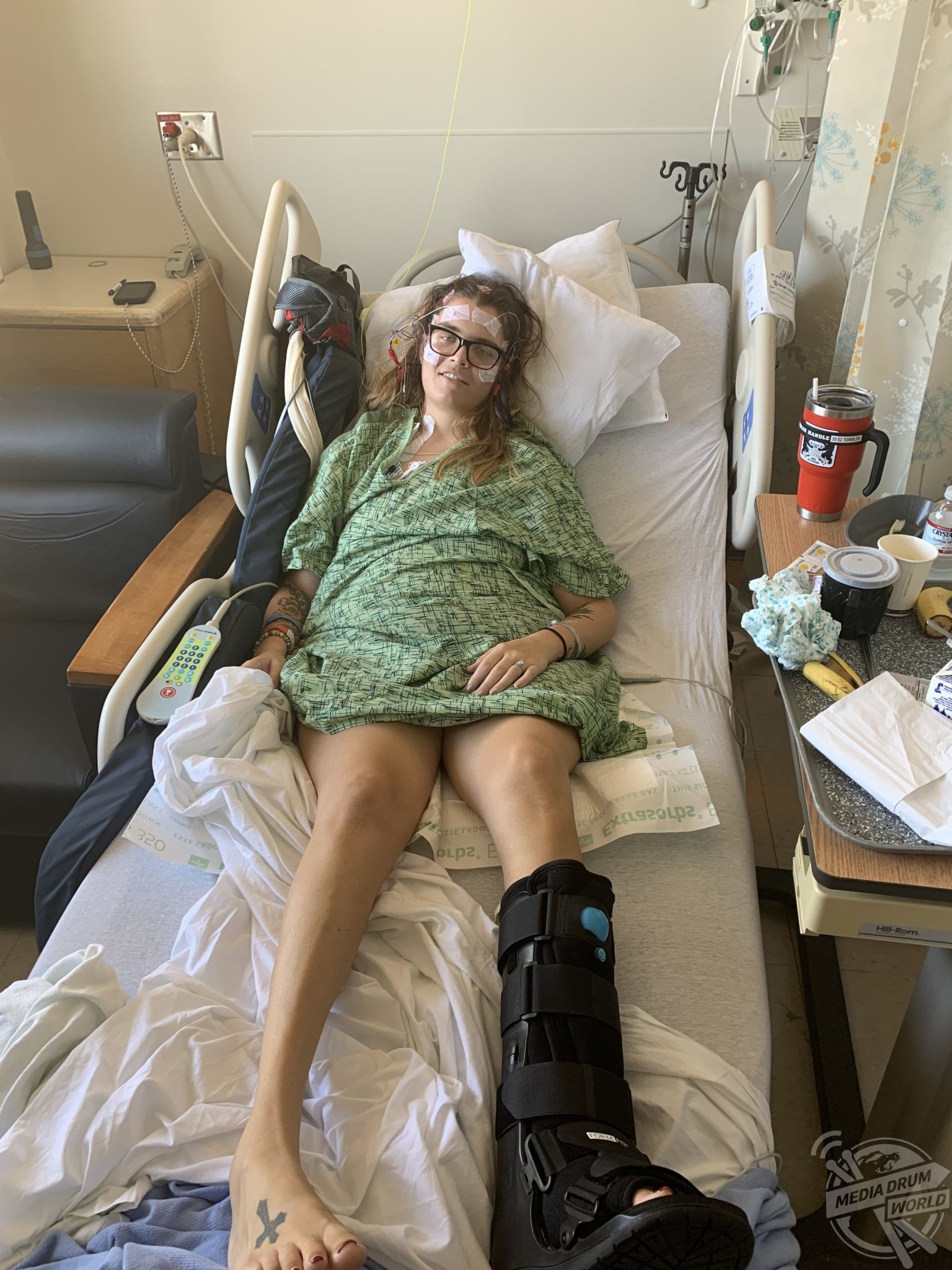
When Samantha Redfield (30) from Angels Camp, California, USA, suddenly started to experience symptoms of stiffness and numbness in her right hand in October 2019, she knew something was wrong.
Over two weeks, the numbness Samantha was feeling spread to her upper right lip and she struggled to feed herself with a fork without dropping it.

Her symptoms escalated and on October 25, she suffered a seizure and she was rushed to A&E where a doctor ordered blood tests and MRI scans, which all came back clear. After being discharged from the hospital and given the all clear, Samantha can’t really fully remember what happened to her as her health rapidly declined.
From speaking to her family and her husband, Codey (40) Samantha knew that she started to hallucinate and she believed that her two sisters, Katie (29) and Danielle (20) had died and that the Mexican Cartel were hunting her and waiting outside her house.
As well as this, she struggled to talk, write and read and even stayed awake for 10 days straight. On November 5, Samantha’s family took her back to the neurologist who misdiagnosed her with schizophrenia and the very next day she went to see a psychiatrist accompanied by her family.

The psychiatrist told Samantha’s family that she did not have schizophrenia and urged them to take her to A&E immediately as she was seriously ill. Samantha was in hospital for two weeks where after countless tests and a spinal tap, she was diagnosed with anti NMDA receptor encephalitis, a rare neurological autoimmune condition which causes inflammation of the brain and which can cause traumatic symptoms similar to the ones that Samantha was experiencing.
Samantha underwent plasma treatment called plasmapheresis which finally brought her out of her psychosis. Samantha is about to undergo IVIG infusions once a month for the next six months to a year to prevent the 20 to 30 per cent chance of relapse. In the meantime, Samantha must take it easy; she’s put her career in marketing on hold whilst she gets better due to her limited energy and hasn’t had a seizure since she was in hospital.
“I knew something was wrong, I quickly became anxious and worried. These symptoms came on quickly over a two-week period just prior to my first seizure,” said Samantha.
“I remember being at a restaurant with my dad and telling him to watch this — I could feel when my hand was about to seize up — I picked up the fork with food on it and before I brought it to my mouth, my hand gave away, dropping the fork and food hit the table, we weren’t sure what to think.
“These symptoms continued to escalate and a week after the fork incident I had my seizure. We would eventually find out these symptoms on the right side of my body were caused by swelling in the left side of my brain.
“I had blood work and an MRI done in the emergency room following the hours of my first seizure, to have them come back clear was honestly scary as it left us with no answers as to what had caused the seizure. Unfortunately, the days following with additional MRIs, EEGs and blood work were a blur. My health quickly started to deteriorate and do not remember much or if any of these tests.

“The hallucinations that I do somewhat remember were thinking I lost loved ones, I remember sobbing thinking two of my sisters had died. I also remember bits and pieces of being incredibly scared that the Mexican Cartel was hunting me, that they were outside our home. I remember very little.
“There is what I believe a good two weeks where I remember nothing. I would be extremely happy one moment and a wreck the next. I had trouble speaking, I couldn’t write or read. I was told I stayed awake for ten days straight.
“My health deteriorated quickly. After another visit to the neurologist I was misdiagnosed as schizophrenic and was referred to see a psychiatrist. My dad scheduled an appointment with a psychiatrist the very next day.

“I’ve been told the psychiatrist said that this is not schizophrenia, she understood I was a healthy happy 29-year-old only weeks before, she knew something was wrong. She recommended my family get me to an emergency room immediately to get admitted. My parents did just that.
“This psychiatrist is the reason we ended up admitted at UC Davis Medical Centre where my life would be saved. To simply put it, my body was attacking my brain and my body was fighting for its life.
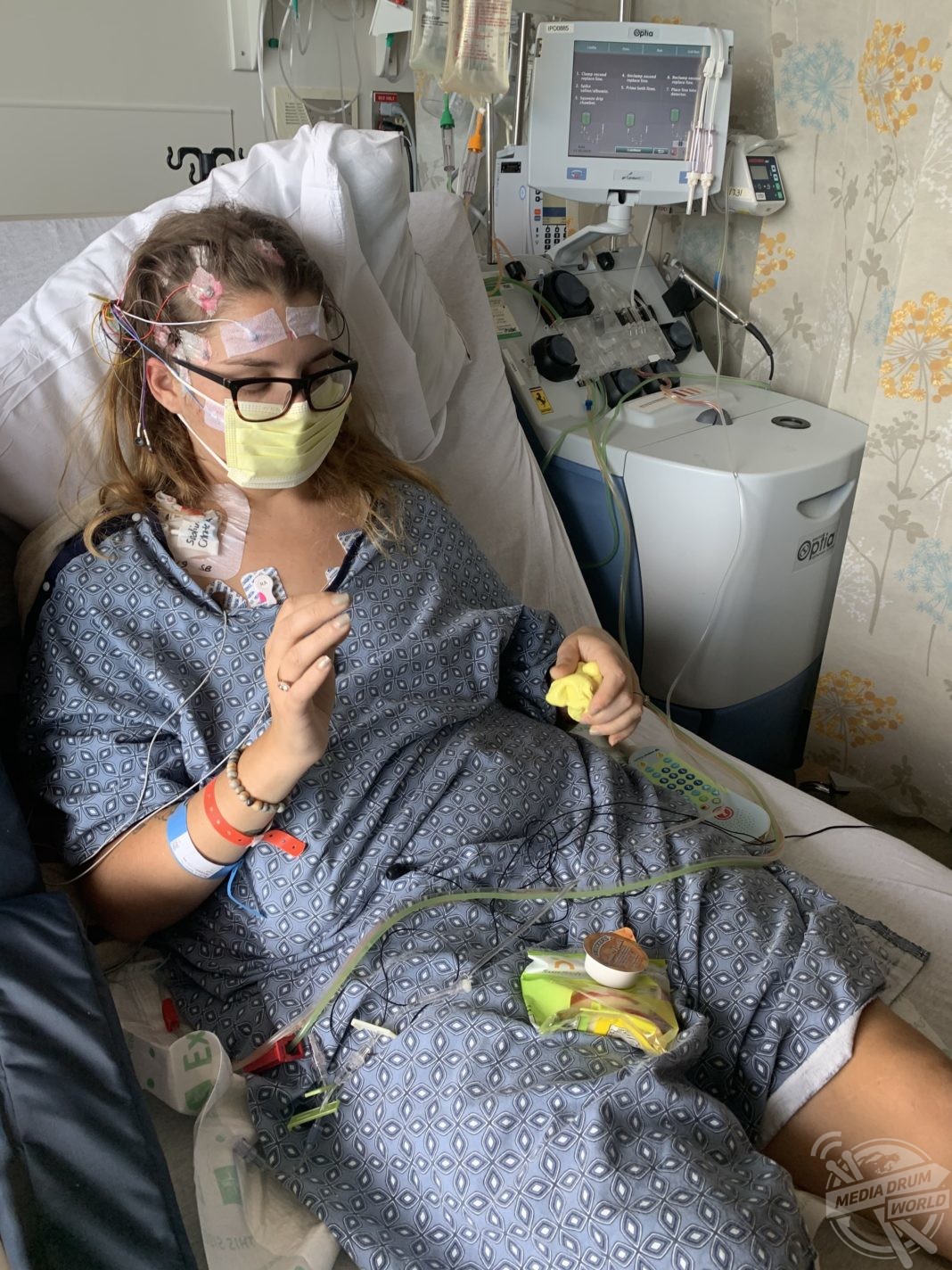
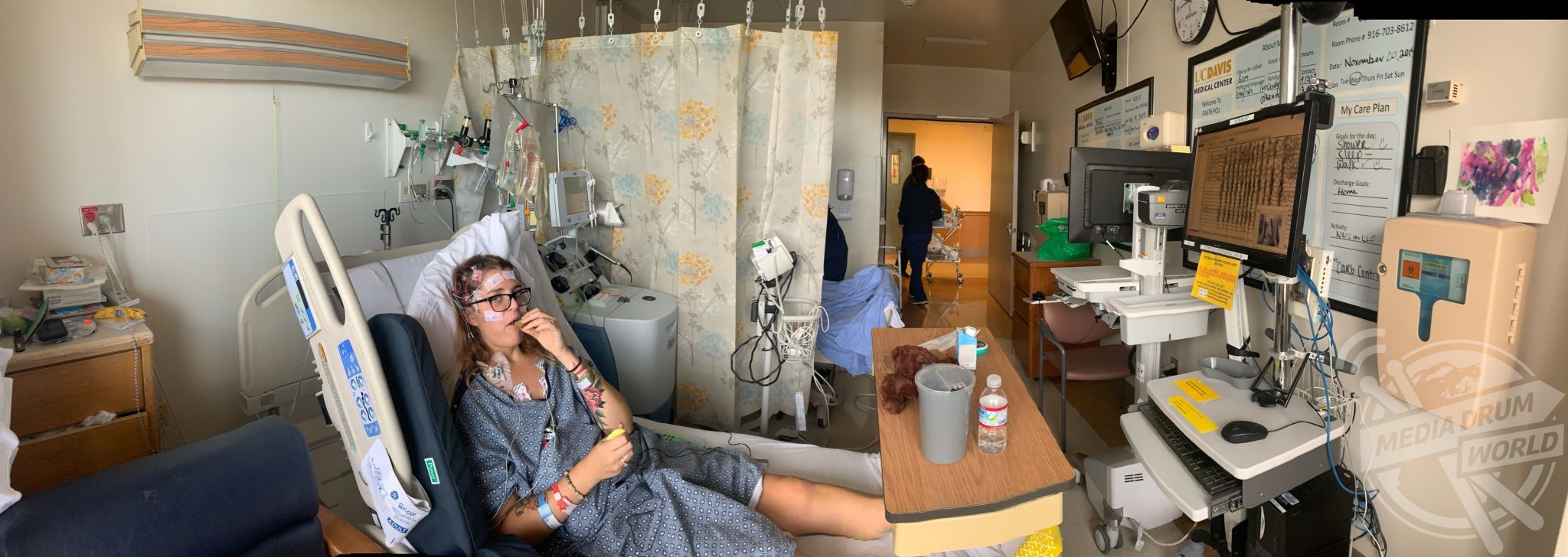
“The doctors turned to an aggressive treatment of plasma exchanges that truly saved my life and brought me out of psychosis. They inserted a catheter near my collar bone. Every other day a specialist would come in with a machine and bottles of plasma. This machine would take my blood into the machine where it would separate my plasma from my red blood cells.
“The machine would then mix my plasma with the fresh plasma and inject it back into my body. This was a two-hour process that happened every other day, five times. By the second or third treatment I started to come out of my state of psychosis.
“Anti NMDA receptor encephalitis is a rare auto immune disease. We all have antibodies that are part of our immune system that protect us from germs and infections. In my case, my antibodies were not working correctly, and they turned on my body and attacked the NMDA receptors in my brain. NMDA receptors are responsible for a lot of our daily activity like human interaction, our memories, judgement and so much more.”
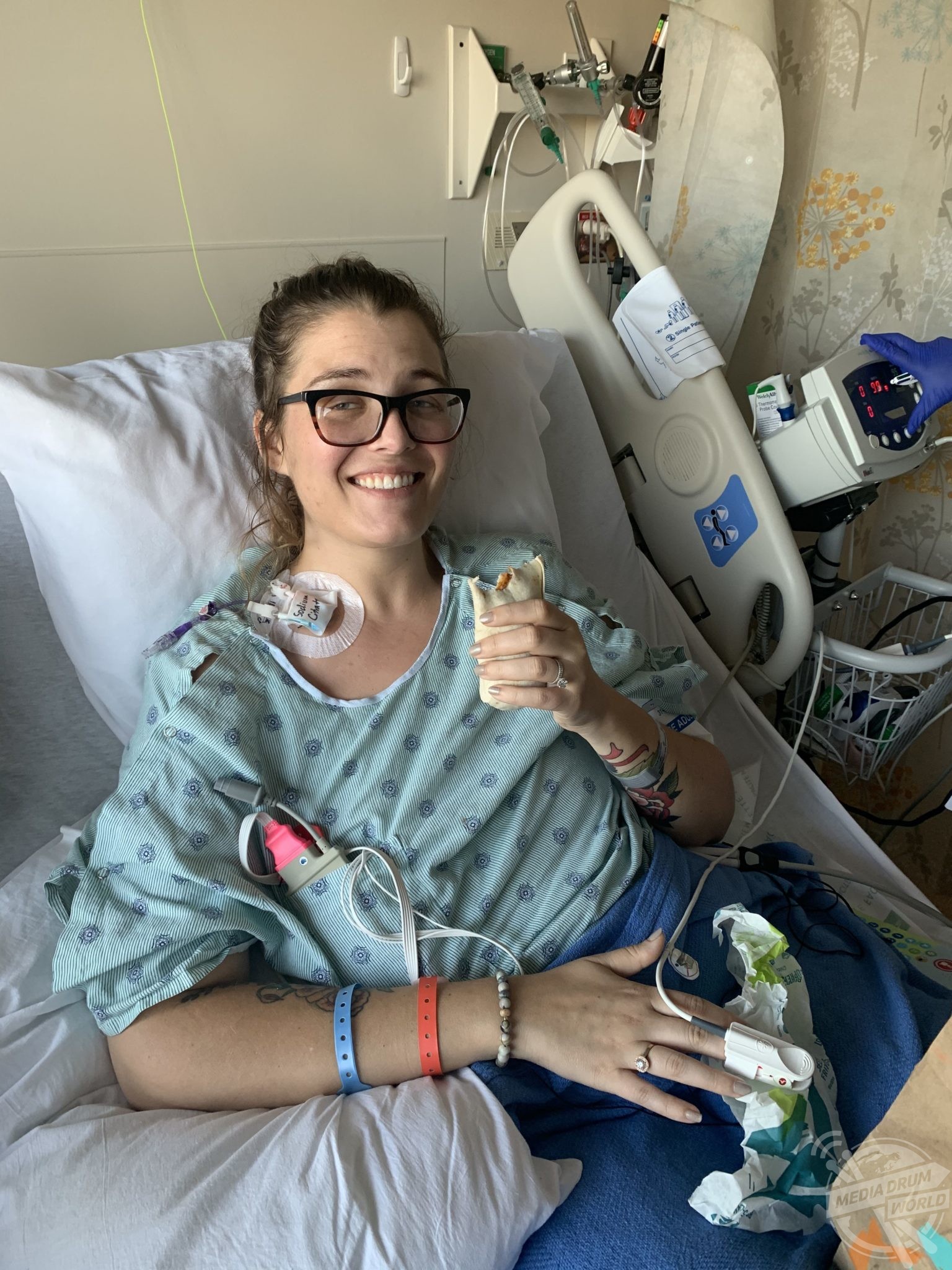
Samantha is still in recovery from her terrifying ordeal but says the moment she came out of her blacked out state in hospital she knew she had to spread the word and raise awareness of anti NMDA receptor encephalitis, which is so often misdiagnosed for a mental health condition.
“Each day is better. My body allows me about four hours of energy a day so the things I do each day are limited still,” she said.
“I can’t drive due to the seizures and with little energy am unable to work so a lot of my time is spent with friends and family or binge watching my favourite shows. I still have a long road ahead of healing and have to remind myself daily to take it easy.
“I’ll start IVIG (antibody) infusions once a month (two days in a row) for at least six months to possibly a year. My new neurologist says there is a twenty to thirty per cent chance of relapse, but we are hopeful IVIG will lessen those chances.

“When I finally ‘woke up’ from my blacked out days and started to understand the rareness of my auto immune disease and how many people go misdiagnosed I felt passionate to use social media as a platform to help raise awareness about anti NMDA receptor encephalitis in hopes that it’ll save a life.
“I am so thankful for the ability to share my story and raise awareness through it, in hopes of saving a life — many are misdiagnosed, not treated and trapped in their own bodies and mental health hospitals.
“Take care of yourself, be gentle with yourself, don’t apologise for something that’s out of your control. You can’t rush healing.”
For more information see www.instagram.com/samantha.raggio.redfield






