By Liana Jacob
MEET THE brave two-and-a-half-year-old boy who cried for FIFTEEN HOURS STRAIGHT because of a rare form of epilepsy which saw him endure SIX SEIZURES in SIX MONTHS.
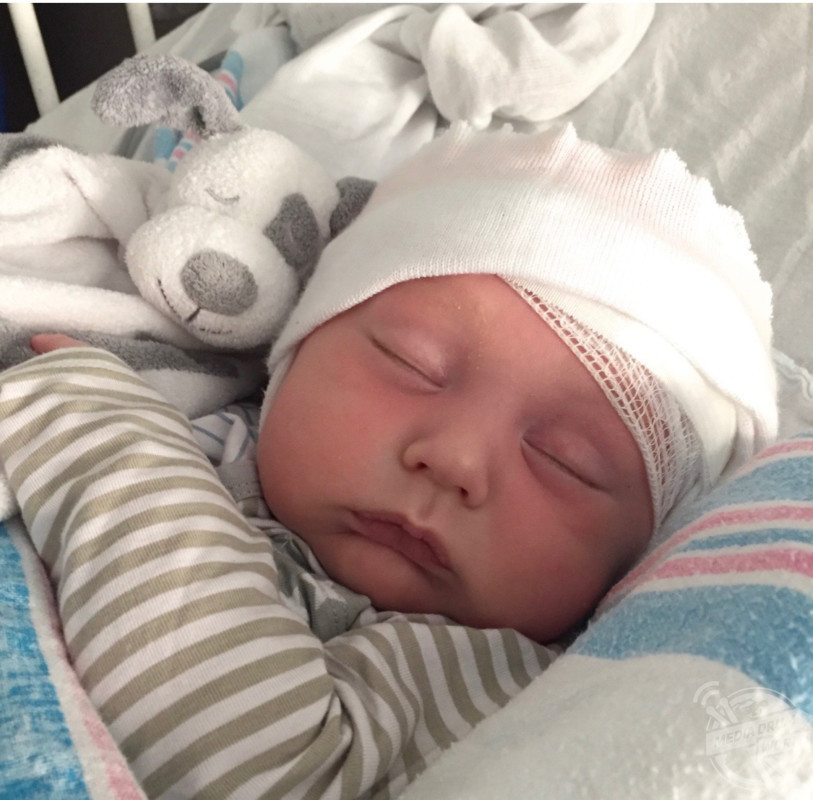
Special needs advocate and mum-of-two, Leah Trotter (30), from Georgia, USA, was over the moon when she gave birth to her son, Jack, in July 2016. Despite undergoing a normal labour, a day after he was taken home, Jack began crying consistently and his cries intensified, and he became inconsolable.

MDWfeatures / Leah Trotter
Initially Leah was calm and wasn’t worried; she rocked him and tried to soothe him, thinking he would feel better soon. The next day, Leah and her husband took Jack to his routine follow-up with his paediatrician, but Jack had still not stopped crying – Jack had been crying for 15 hours consistently.
Leah expressed her growing concern at the paediatrician’s office, who informed her that it may be gas or reflux related, so they were sent home. Jack had finally stopped crying at 8pm that evening, but he stopped nursing and gradually stopped eating. He began exhibiting strange behaviour like random movements of his arms, legs and head. The paediatrician referred him to the local hospital who then recommended they see a neurologist.
MDWfeatures / Leah Trotter
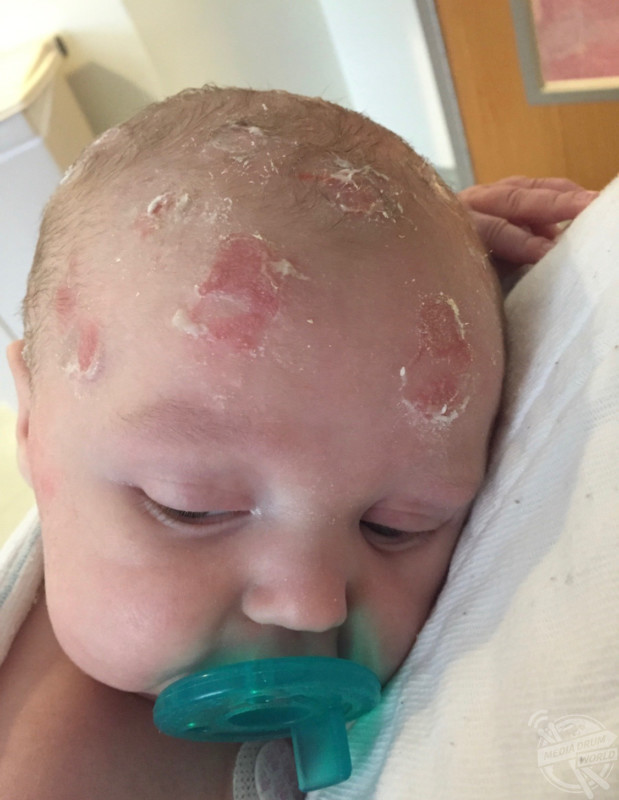
Three months later, Jack was stabilised and admitted to hospital again, where he began having gelastic (laughing) and dacrystic (crying) seizures, then rushed for an MRI scan. Following the scan, a neurologist diagnosed Jack with Mitochondrial disease and that he was likely to die due to brain damage.
This turned out to be a misdiagnosis, as in December 2016, Jack was correctly diagnosed with Pyridoxine Dependent Epilepsy (PDE), a rare cause of stubborn, difficult to control, (intractable) seizures appearing in newborns, infants and occasionally older children. Over 200 cases have been reported in medical literature.
MDWfeatures / Leah Trotter
Jack has had numerous types of seizures in the first six months of his life such as; tonic-clonic, partial, focal, absence, gelatic, dacrystic and even some where he just has constant hiccups.
“I was on top of the world when Jack was born. He was perfect at eight pounds and three ounces, 22 inches long. He nursed perfectly right off the bat,” Leah said.

MDWfeatures / Leah Trotter
“I had Jack on a Saturday morning and we went home on Monday afternoon. Everything was perfect; he ate well, he slept well, he was an easy and happy baby.
“I was so blind to the true hardships in life and without warning, my life changed in an instant. Did I even blink? Had I been dreaming all along?

MDWfeatures / Leah Trotter
“Tuesday evening, late, Jack started crying. His crying intensified, and he became inconsolable. I was so calm and patient and didn’t feel the least bit worried.
“I rocked him, loved him and knew he would feel better soon. We had our routine follow-up with his paediatrician on Wednesday.

MDWfeatures / Leah Trotter
“Jack had still not stopped crying by that time. No exaggeration, Jack cried for fifteen hours straight. He cried the entire time at the paediatrician’s office and I expressed my concern.
“We went home, and the crying did not stop until about 8pm that evening. Jack had still been eating throughout all the crying, but then he stopped nursing.

MDWfeatures / Leah Trotter
“I pumped and tried the bottle. Gradually throughout the night he basically just stopped eating, but he eventually stopped crying as well.
“As the crying stopped, something new started. I cannot explain it, although I have told the story to more doctors than I can count.

MDWfeatures / Leah Trotter
“Jack did not look quite right after the crying stopped. Keep in mind, he was barely five-days-old at this time so it was hard to say if he was just brand new or if he was acting strange.
“Babies are strange; they have strange movements. But something was neurologically not right, and I knew it.

MDWfeatures / Leah Trotter
“He did not look like he was seizing (not in the sense that I thought a seizure looked like at that time at least), but something told me he was having little seizures.
“He was slightly shaking, jittery as they called it in the hospital, and then he would startle and throw his left arm out and turn his head to the left simultaneously.

MDWfeatures / Leah Trotter
“There is no way to explain this act, you just had to see it. I tried everything to see if I was imaging it or if something wasn’t right.
“My mum helped me give him a little sponge bath. He seemed rigid. I was done. I called the paediatrician and we went back in the next morning. Jack was just five-days-old.”

MDWfeatures / Leah Trotter
Despite Leah’s worry, she says the staff at the hospital didn’t take her concern very seriously, until a nurse approached them and noticed something wasn’t right.
“Before I knew it there were six or seven nurses in the room, all crowded around Jack trying to help him and my husband and I faded into the background as they worked,” Leah said.

MDWfeatures / Leah Trotter
“I have never been so scared in my life. It was soon decided that Jack needed to be sent to Children’s Healthcare of Atlanta (CHOA), the best paediatric specialists in our state.
“I was terrified because this confirmed that something bad was happening to our newborn son.
MDWfeatures / Leah Trotter
“Jack only got worse and was in and out of the hospital with hard to control seizures, put on so many medications, and still no answers. When he was almost three-months-old, he was in status again and admitted to the PICU.
“During this visit, he began having gelastic and dacrystic seizures and was rushed for an MRI. After this MRI, a Neurologist told us that Jack had Mitochondrial Disease and his brain has begun to atrophy and would continue to until he died.

MDWfeatures / Leah Trotter
“They told us there was no hope, but they sent many genetic tests off that day as well. Jack was still in and out of the hospital with hard to control seizures for the next few months.
“A few days later we finally received Jack’s accurate diagnosis as his genetics had come back. His treatment for the first six months of his life had been all wrong, almost detrimental to him.

MDWfeatures / Leah Trotter
“We immediately saw a neurologist, genetics, nutrition, all the specialists we needed to get Jack on the right track.
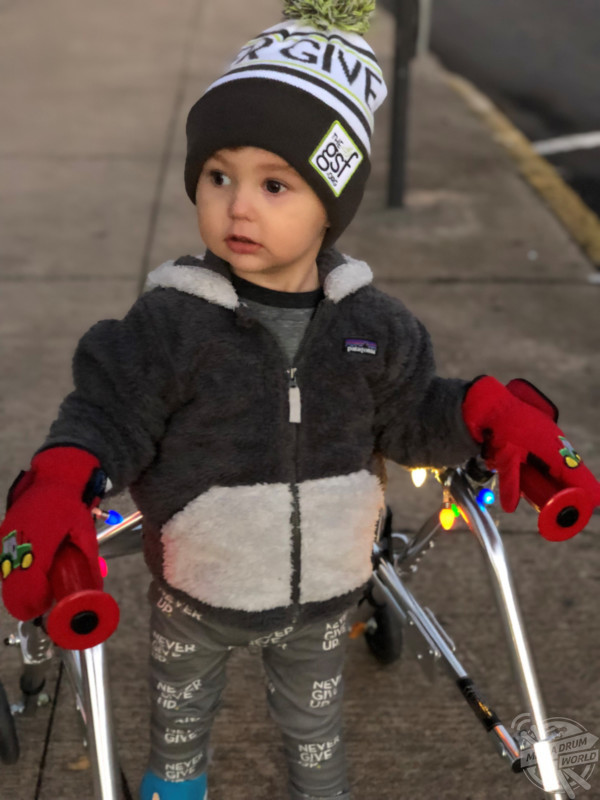
“We have been working so hard ever since with six therapies per week for Jack and lots of work at home. He still has many delays and a few new diagnoses, but he has a great quality of life.
“Everyone has been incredibly supportive throughout the entire journey and still are. We could not have made it through any of this without our amazing support system.
“I have a few things that I am incredibly passionate about and want to work on in the future. First and foremost, I want PDE added to the new-born screening.
“We went through six months of hell and our son almost died from a treatable condition that could be tested at birth. So, that is my first order of business.
“I try to advocate through social media platforms for PDE and I have since helped a mother in Brazil obtain access to the specialists necessary to treat her daughter with PDE.
“I would like other mothers in similar situations to know that they control the narrative. Don’t let a doctor dictate the way you feel about the diagnosis being given to your child.
“I hope that all mothers faced with these situations won’t become overwhelmed with the heavy diagnosis and medical terminology being thrown around, but instead will use the opportunity to rise up and make the best quality of life for their child.”









