By Alyce Collins
STEROIDS caused this woman’s eczema to spread like WILDFIRE and forced her to MOVE BACK IN WITH HER PARENTS – and she says UK doctors are handing them out ‘like sweets’.
Graphic designer, Holly Broome (24), originally from Gloucestershire and now living in London, UK, was born with atopic dermatitis but it wasn’t discovered until she was two weeks old, and from then it became progressively worse.
Holly remembers taking oral steroids to help her eczema, but as the problem grew worse, she had to be hospitalised and wrapped in bandages at night to prevent scratching – although this didn’t work and only irritated her skin more. Thankfully by the time she reached her teens her eczema had become better and she wasn’t using topical steroids.

Unfortunately, during a difficult period in her life, Holly became incredibly stressed during university in 2017 which triggered an eczema flare on her back, legs and arms. Holly went to a GP but was only told it wasn’t ‘that bad’, to moisturise more often and use a stronger topical steroid.
Holly continued using Eumovate, a strong topical steroid, on the affected areas as well as moisturising twice a day and taking cool showers. However, during the summer of 2017, Holly’s skin seemed to be getting worse and the rash on her back was spreading all over her torso, arms and face. She was constantly sore, her skin radiated heat and it hurt to shower.
As Holly continually returned to her GP, she was prescribed more steroids, despite her eczema spreading and becoming more painful after using steroids. By that winter, more than 70 per cent of Holly’s body was covered in eczema.
After trying an eczema diet, consisting of rice, chicken and cabbage, and seeing no improvement, Holly read about topical steroid withdrawal (TSW) and was horrified by the damage it could do, but initially she refused to believe that was what she had until researching it further.
“I’ve struggled with eczema my whole life after it presented itself when I was two weeks old and got steadily worse until I was hospitalised aged five,” said Holly.
“I was wet wrapped in steroid bandages and was constantly on oral steroids and antibiotics. I remember waking up every night and scratching until my bandages fell off. My skin never responded particularly well to steroids, it was always so red and burning hot.
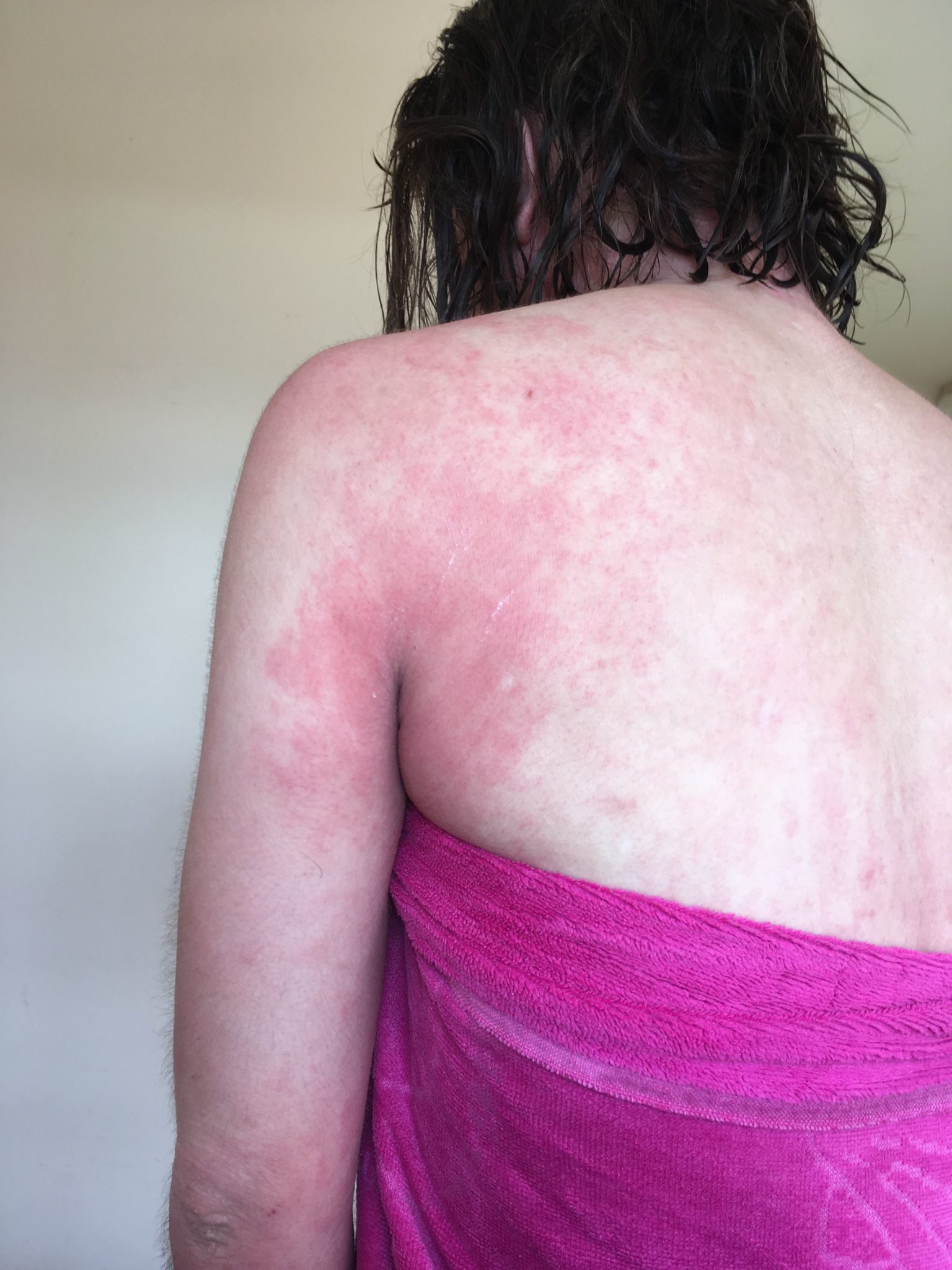
“Thankfully my skin calmed down for most of my teenage years and I only had small patches of eczema. My skin was generally dry but nothing too uncomfortable.
“I went through an incredibly stressful period whilst at university. I lived in a shared house with people who made my life difficult and at the same time my mum was diagnosed with a brain tumour. Stress is my biggest trigger so throughout this stressful period my skin kept flaring, and I did what anyone else with eczema would do: I went to the doctors.
“The GP took a quick look at my skin, which by that point was the worst it had been in years, and told me I wasn’t moisturising enough, that I wasn’t using a strong enough steroid and she said ‘it’s not that bad, I’ve seen worse’. I left that appointment feeling completely deflated.
“She had dismissed my suffering based on other people’s eczema which was completely unfair. She passed the blame onto me, claiming I wasn’t managing my eczema properly. I was moisturising twice a day, applying steroids once a day, and taking the usual precautions such as cool showers, but apparently this wasn’t enough. Using Eumovate, my skin did calm down, but only a few months after I graduated it came back again.
“While interning in London, my skin was getting worse as the rash on my back started spreading like wildfire onto my torso, all up my arms and onto my face – somewhere that hadn’t been affected since I was little. I struggled to get out of bed in the morning, my skin oozed fluid all over the bed sheets, I was flaking, and my skin felt hot to touch.
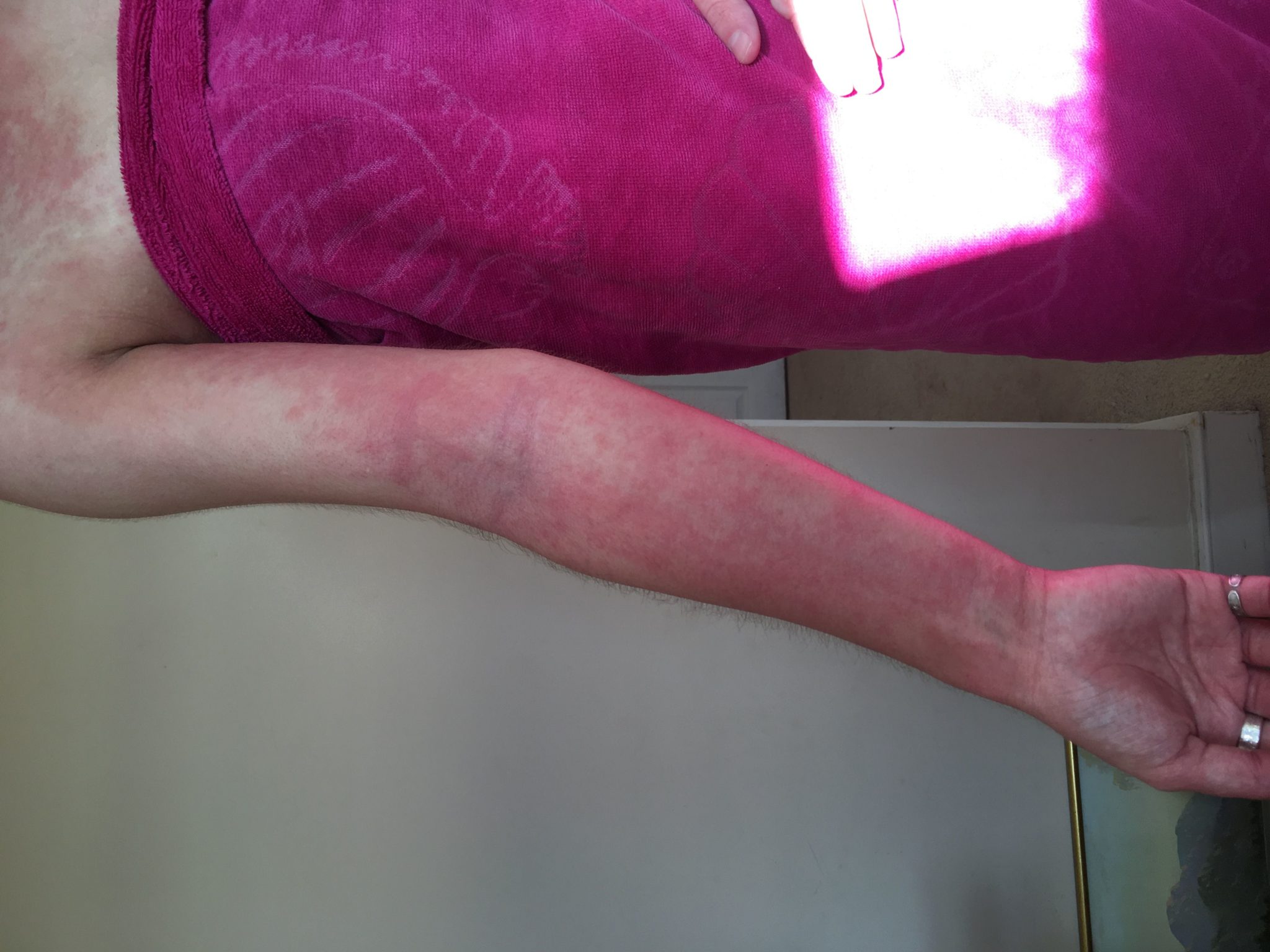
“I got an appointment with my childhood GP and he prescribed me oral steroids, antibiotics and more Eumovate. Thankfully this was enough to calm my skin down in time for graduation but by winter my skin was bad again.
By the start of 2018, oral and topical steroids had no effect on Holly’s skin, and she started trying new methods of healing, but nothing helped. After hearing about TSW in February, Holly researched the condition before stopping all steroid use on April 19, 2018, after trying to taper down her usage for a month to no avail.
TSW dramatically resulted in Holly moving back in with her parents so she could be taken care of six weeks into her withdrawal. Holly felt so desperate for something to help and at the end of June 2018 she discovered no moisture treatment (NMT), which helps the skin produce its own moisture.
“Whilst reading the Eczema Diet book, I came across a term I’d never heard before. That was TSW. I found horrifying images of people whose skin was unlike anything I’d seen before. Initially I was in denial that TSW was what I had, I used steroids as the doctors instructed so I couldn’t be that addicted to them. I was wrong. I couldn’t possibly have been prepared for how bad my skin would get,” she said.

“I stopped using any kind of steroid in April 2018. Over the next month my skin deteriorated rapidly. I could no longer sleep at night due to night sweats and the constant itch that moved around my body.
“I shed vast layers of skin every night and my boyfriend had to hoover the flat every day, as well as the bed every time I slept in it. Underneath the layers of the skin that were peeling off wasn’t new skin, it was raw, damaged skin that oozed a yellow liquid.
“I could hardly shower anymore due to the pain of the water jets and the towel. Eventually I had to move home with my parents in Gloucestershire as I couldn’t look after myself anymore and needed access to a bath.
“I was now red over 95 per cent of my body, my adrenal gland was messed up and not functioning properly due to its dependence on the synthetic hormones I’d been rubbing onto my skin. I was in an unbelievable amount of discomfort. I didn’t recognise the face in the mirror anymore and I didn’t leave the house for months.
“Eventually I came across the no moisture treatment which involves ceasing the use of any moisturiser, reducing showers to once or twice a week, moderate exercise, reduced water intake. After a few weeks, my skin improved; the redness went right down, my skin stopped oozing and many of my open wounds started healing. By August I was well enough to move back to London and go back to my job.

“Since then my skin has been constantly healing. It still flares every now and then, but I just leave it alone and within days it’s back to normal. I no longer moisturise, and my skin is less dry than when I was moisturising. I stick to one or two cool showers a week and my skin is thanking me for it.”
Holly also talked about how doctors are reluctant to advocate for TSW but she, along with friends she’s made in the TSW community, have started a campaign called Scratch That to raise awareness.
“TSW isn’t currently recognised in the UK but there’s a massive online community of people suffering from this condition,” Holly said.

“I don’t want to claim that I’ve healed my eczema, but I’ve found a way to control the condition which goes against any advice my doctors gave me. Currently, steroids are handed out like sweets with little instruction on how to use them properly or when to stop.
“There’s five of us, myself, Harriet, Louise, Hannah and Laurie who have created the campaign called Scratch That, with the aim of getting this condition the recognition it deserves. As a community we feel lost and unsupported so we’re hoping to change this. The aim is to campaign to get the prescription of topical steroids more controlled and to get topical steroid addiction diagnosed and treated properly.”
To see more, visit https://www.instagram.com/scratchthat.uk/ or go to Holly’s profile at https://www.instagram.com/tsw_hollybee/






