By Rebecca Drew
AN INSPIRATIONAL British student has revealed how she learnt to walk again and is lifting weights in the gym after she was struck down by a terrifying nerve condition that left her bed-bound and unable to breathe independently or do anything for herself.
In April 2017, when student, Jodie Granger (22) from Cornwall, UK, first noticed a gradual change in how her hands and feet felt she didn’t think too much of it until the same sensation started to spread towards the centre of her body and she was finding it tiring to move her arms and legs. This progressed and within the space of a week, Jodie was in hospital with her symptoms getting worse by the day.
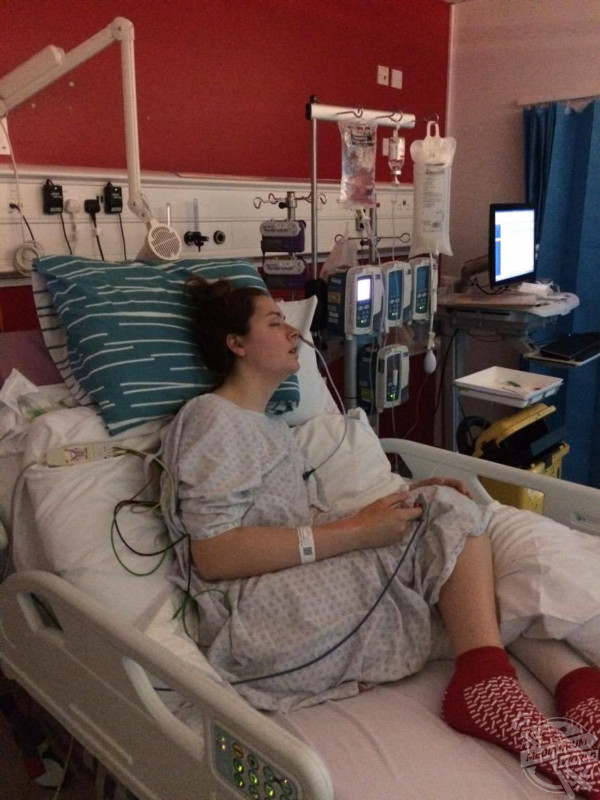
Jodie Granger / MDWfeatures
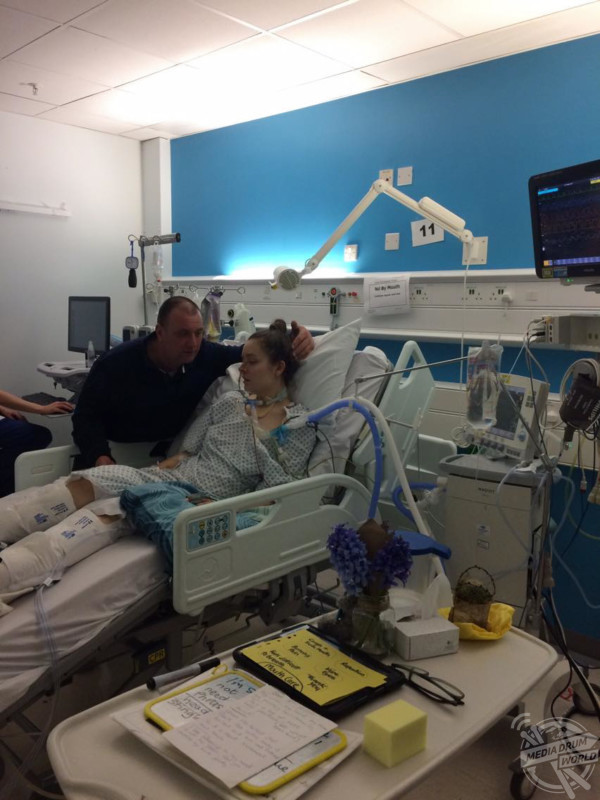
Jodie was diagnosed with Guillain-Barré syndrome (GBS) and whilst in intensive care, all of her physical needs were being met by the people looking after her at King’s College Hospital’s Intensive Care Unit. Jodie had a tracheostomy so that she could be fitted with a ventilator to allow her to breathe which left her unable to talk during this time.
Jodie was in hospital for eight weeks and could walk again after six thanks to intensive physiotherapy, and more recently, she has been lifting 75kg weights in the gym to build her strength, she discussed her diagnosis and recovery.
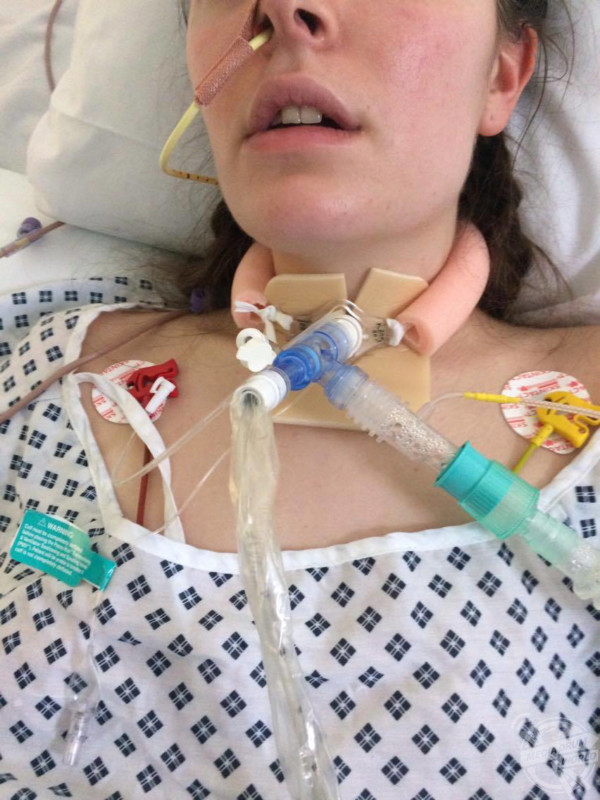
Jodie Granger / MDWfeatures
“It happened quite slowly to begin with, gradually I felt the change of sensation in my hands and feet and it just spread towards the centre of my body, and it got harder to move my limbs or felt like more of an effort, including walking especially,” she said.
“I had severe pins and needles, which felt like burning, and muscle weakness, numbness on the skin.

Jodie Granger / mediadrumworld.com
“The time frame between me starting to feel ill, and it gradually getting worse, happened in the space of a week. By then I was in hospital still on a downward slope, and the symptoms were picking up momentum, each day was quite a bit different.
“Someone with GBS cannot control body movement that they previously had control over, and often a person has to be mechanically ventilated, leading to a dependence care for all aspects of life including feeding, hygiene etc, and will undergo treatment and intensive physiotherapy to combat the effects of GBS.

Jodie Granger / MDWfeatures
“Physically all of my needs were being met by other people looking after me on intensive care, as I couldn’t move properly and was bed-bound. I had a tracheotomy performed on me, meaning I was unable to talk.
“At this point I was probably at my most vulnerable physically and mentally. I was in so much pain and discomfort that it’s almost impossible to explain, on top of the need to communicate these things at the time but not doing so quick enough or effectively enough as you have to try and spell things out one letter at a time.

Jodie Granger / MDWfeatures
“You have to be weaned off the ventilator for one thing, by building up your tolerance of having less assistance from the ventilator machine and increasing your control and effort you can put in to be able to support your own breathing via a speech and language therapist.
“You also have to undergo physio as movement to limbs start to come back, including fine-tuned movement that you go through with an occupational therapist, and other wider ranges of strength and mobility focused by the physiotherapists.”
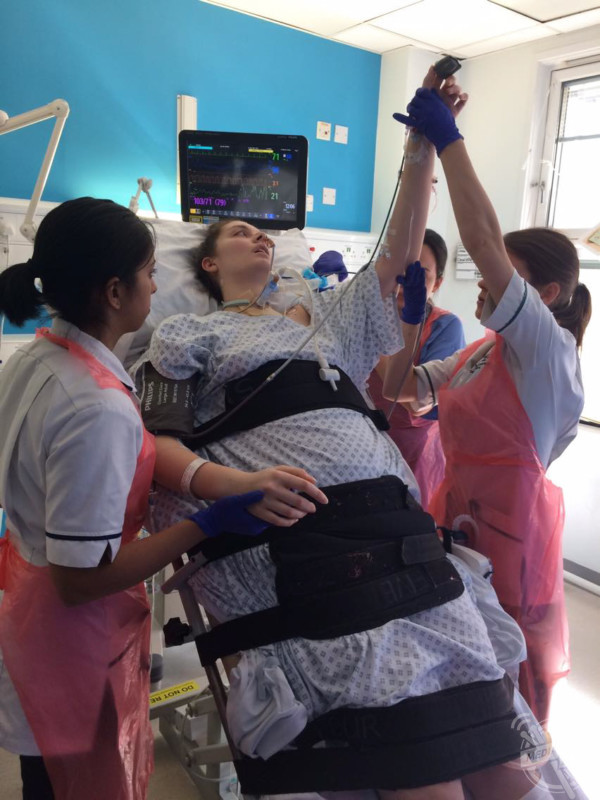
Jodie Granger / MDWfeatures
GBS is a very rare condition that affects the nerves. It mainly affects the feet, hands and limbs which can cause numbness, weakness and pain. Early symptoms can continue to get worse over the days or weeks and severe cases can cause paralysis and difficulty breathing and/or swallowing.
It is thought to be caused by a problem with the immune system which attacks germs or infections in the body but in people with GBS, something goes wrong and the immune system starts to attack and damage the nerves.
The year after Jodie’s diagnosis and treatment was very difficult for her as she readjusted to life back at Goldsmiths University, London whilst also coming to terms with the physical and mental trauma she had been put through.
“How I’m feeling about myself now is a hard question I may have to come back to; on one hand it is a fascinating story and journey, in such a short period of time, in which I am proud of myself of achieving, and on another hand, I still have a lot of things to deal with mentally and physically,” she explained.
“The following year was a struggle, in terms of getting back to my uni life which I was fully entitled to do, to re-take second year, but the bureaucracy was incredibly difficult, on top of the memories, physical and mental trauma I had to deal with, and still feel I am dealing with.

Jodie Granger / MDWfeatures
“I think the most difficult is this aspect of trying to make sense of or understanding this particular trauma. It was luckily not as long as other GBS/CIDP cases, but it was very severe in a short space of time.
“The experience of not being able to talk or move properly, alongside feeling neuropathic pain, and have all kinds of procedures to go through, whilst trying to stay calm, and live in a hospital, and try to get better as soon as you can.”
Jodie says that her battle with GBS has brought her closer to her loved ones and she shared her words of support to other sufferers.
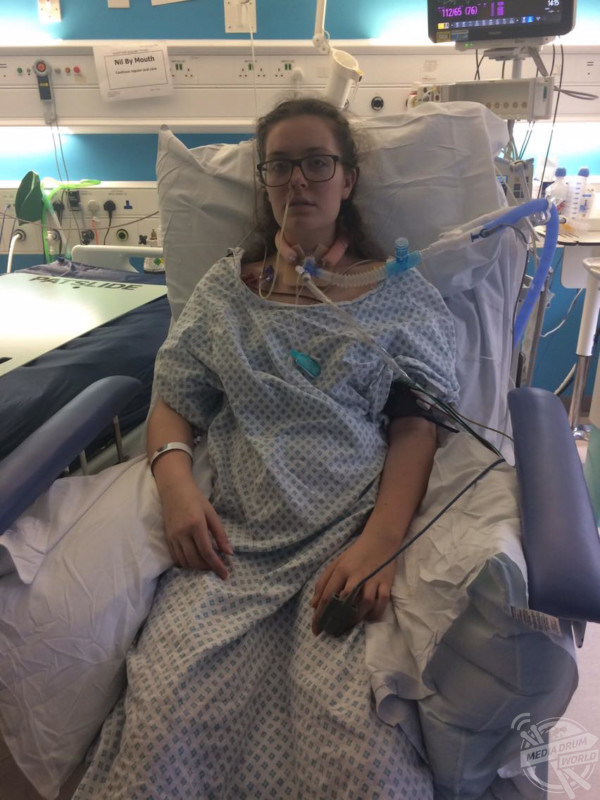
Jodie Granger / MDWfeatures
“Friends and family are amazed by it, simply put. Very happy that I turned out ok in the end, because we were all quite scared to begin with; no one knew what was on the road ahead, so when I started to get better that was something to hold onto and support, as I kept improving every day,” she added.
“I had so many people visit me, almost nearly every day a friend or group of friends or family members would have come to London to be with me, so that was a positive distraction from the mundane routine of being in the same room night and day.

“My parents had been with me practically the whole time, so they’ve seen everything and actually experienced it all alongside with me, which has made us closer.
“I would advise to someone that I understand the immense frustration of being unable to communicate and/or control bodily movement. I understand the pain of not knowing what lies ahead, of feeling as far away from your previous life as you may have felt so far, whether or not you’ll ever get back to that.
“It is extremely tough, but if you engage as much as you can with each step, keeping track of just the smallest improvements that happen every day, eventually you’ll accumulate more and more control, you will have this perspective gained, which a lot of people may not gain throughout their entire lives.
Jodie Granger / MDWfeatures
“You will see how the important the health system is, how it operates, how it needs to be protected and supported in every sense, and unfortunately how pressed people working in the NHS are, but how much they care for their patients.
“People around you are there to give you so much love, and will do anything to alleviate even the smallest amounts of discomfort, and there is no shame in asking for such; some of the smallest things make the biggest difference.”
For more information see www.mediadrumworld.com







